Malaria
The Secret Immigrant
by Ken W. Watson
When ships first started plying their way to the New World with immigrants from Europe, and later, slaves from Africa, there were stowaways, or perhaps better described as hitchhikers, on board. From Africa came the parasite, Plasmodium falciparum (P.falciparum), the deadly tropical form
of malaria. From Europe came the parasite, Plasmodium vivax (P.vivax), a less deadly temperate form of malaria. By the mid-1600s, both were firmly established in the southern portions of North America and P.vivax was established in some of the more populated northern areas of today’s U.S.
To understand the spread of malaria in North America, and eventually to the Rideau Canal, one has to understand what malaria actually is. It is a parasite that needs two hosts to survive, a particular type of mosquito and a human. The life cycle of the malaria parasite starts when a malaria-carrying mosquito bites a human. The parasites (as sporozoites) head to the liver and proceed to incubate. The sporozoites multiply and, when sufficient numbers are reached, head out to invade red blood cells and produce merozoites.
These merozoites multiply and eventually burst the red blood cells, producing the classic chills and fever symptoms in the victim. It is at this stage that an Anopheles mosquito can pick up the parasites when taking blood from a human with the disease. Once back in the mosquito, the merozoites develop into male and female gametocytes. These gametocytes fuse in the mosquito’s gut (stomach) and produce sporozoites, which head into the mosquito’s salivary glands, ready to be injected into the next human victim, and start the cycle all over again.
P.vivax was present in temperate climates because it had developed a survival strategy to live through periods when mosquitoes weren’t out
and biting (i.e. winter). It can stay in the liver for months, sometimes years, before heading back out into the bloodstream to be picked up by a biting mosquito. P. falciparum on the other hand, doesn’t do this, and so it must depend on a constant source of mosquitoes (i.e. a year-round warm climate) to maintain the cycle.
| |
 |
Anopheles Mosquito
An Anopheles mosquito (an Anopheles Freeborni in this photo) sucks up a blood meal from an unsuspecting human sleeping at night. During this process it can either acquire or deliver the malaria parasite. Image from the U.S. Centre for Disease Control.
|
The malaria parasite is carried by a specific type of mosquito, a female Anopheles mosquito (generally Anopheles quadrimaculatus in eastern North America – one of 60 different species of mosquito in Ontario). The Anopheles is a night-biting mosquito, and, unlike most other species of mosquito, has the ability to take multiple blood meals. This allows it to pick up the malaria parasite and then spread it back to humans. But it’s a game of odds. With only a few humans scattered far and wide, the chances of maintaining the cycle (enough humans and mosquitoes infected) is low. But when a group of infected humans is together in an area frequented by the Anopheles mosquito, the cycle can be maintained.
P.vivax followed expanding human populations within the range of the Anopheles mosquito. It had established itself in Ontario by the mid-1700s. It was most commonly referred to as ague, fever and ague, or intermittent fever (ague generally refers to alternating chills, fever, and sweating). Its association with marsh land (where the Anopheles mosquito was most
prevalent) gave rise to other names such as Marsh Fever, Swamp Fever and
Lake Fever.
P.vivax is generally a benign form of malaria. It only infects new (immature) blood cells and while people get sick, they generally don’t die. On the other hand, tropical malaria, P.falciparum, infects a much higher percentage of the host’s red blood cells and reproduces much faster than P.vivax, so it can have a significant mortality rate. We do have evidence that P.vivax can kill, although the exact reasons are still shrouded in mystery. For instance, in the marshes of Kent, England, a major habitat for the Anopheles mosquito, death rates in the 17th and 18th centuries were much higher than for the general population, a result of the almost ubiquitous P.vivax malaria, known locally as Marsh Fever.
When the Erie Canal was being built, work in 1819 was halted in the area of Montezuma’s Swamp (west of Syracuse, New York) due to a large outbreak of malaria. Stories have grown over time to say that 1,000 men died in this area. That number is likely greatly exaggerated, but men did die and it foreshadowed the problem with malaria that was to plague the Rideau region less than 10 years later.
Malaria on the Rideau
In 1826, before construction started on the Rideau Canal, malaria was well established in both Kingston and Perth. Reverend William Bell, living in Perth, was busy procuring Quinine, the main prophylactic and cure for the disease. Contemporary letters and accounts indicate that most newcomers to the country suffered from ague. In 1825, immigrants brought into Upper Canada by Peter Robinson spent some time in Kingston, most suffering from ague.
In the northern parts of the Rideau, the low population density and the fact that this was outside
the primary range of the Anopheles mosquito meant that ague was far less prevalent. John Mactaggart noted: “The Ottawa is conceived to be
a very healthy river; the people on its banks are seldom or never sick ; and the Lower Province [Québec] is much freer from distemper than the Upper [Ontario].”
In 1827, construction was starting on the Rideau Canal. Very few people died in 1827 and while there was no mass attack of malaria, it was nonetheless present. We have
a few clues about this in the 1827 records of A.J. Christie, who was hired by Colonel By to provide medical care to the workers along the Rideau.
| |
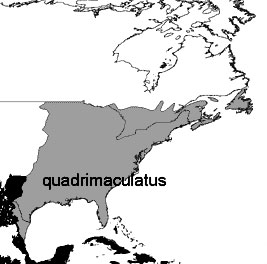 |
Anopheles Range
This is the estimated range today for the Anopheles Quadrimaculatus mosquito. It is present in the southern portions of Ontario. Image from Wikipedia.
|
In his listings of the 1,278 men he treated between May and December
1827, he indicated that a number had fever. This was either “Febris Contd.”
(continued or continuous fever), “Feb. Intermit” (intermittent), or “Feb.Tertian.” Tertian is a fever that recurs every other day. P.vivax malaria causes a
tertian fever so Christie’s Feb.Tertian is almost certainly malaria and odds are
that his Feb.Intermit is malaria as well. Christie’s records show continuous
fevers as generally lasting 6 to 9 days while intermittent and tertian fevers
lasted from 14 to 19 days. While most survived these fevers, Christie noted 5
deaths from continuous fever and none from intermittent or tertian fever.
The vast majority of Christie’s patients had bowel disorders, the most prevalent was diarrhea plus many cases with indigestion and constipation. The causes for these could be many, from e-coli bacteria to intestinal worms. The unusually high mortality from P.vivax along the Rideau may have its root in underlying medical conditions. A person already enfeebled by a medical issue, such as those recorded by Christie, then hit with malaria, could succumb. Christie’s records show that the men suffered from a lot of medical issues.
It is possible, although very unlikely, that tropical malaria, P.falciparum, which does have a significant mortality rate, was present along the Rideau. But it would have had to been re-introduced each year, in numbers high enough to have an infection rate producing deaths. The general evidence, including the fact that P.vivax does appear to be a contributing factor in deaths during that time period in such places such as Kent, England, makes medical issues plus P.vivax malaria the most likely cause of mortality.
By the summer of 1828, work camps were fully established along the Rideau. The exceptional hot weather conditions that summer produced a bumper crop of Anopheles mosquitoes. Malaria severely hit the Rideau and many other parts of Upper Canada. The “sickly season,” as it was already known in Upper Canada, generally spanned six weeks, from the beginning of August to mid-September.
An 1834 handbook for emigrants noted that “In the remarkably hot summer of 1828, the lakes appeared, like fresh water kept long on shipboard, in a state of putrefaction ; and in course of the disengagement which restores their usual limpid purity, threw up a noxious slime. Fever and ague, in almost every part of Upper Canada, followed.”
We also have an often quoted description of the 1828 malaria outbreak by John Mactaggart. He wrote: “In the summer of 1828, the sickness in Upper Canada raged like a plague ; all along the banks of the lakes, nothing but languid fevers; and at the Rideau Canal few could work with fever and ague ; at Jones’s Falls and Kingston Mills, no one was able to carry a draught of water to a friend; doctors and all were laid down together.”
How Many Died?
The 1828 sick records for Jones Falls show the effect of this outbreak.
On August 1 there were 261 men at this worksite. Site abandonment due
to fear of sickness dropped that number to 86 by August 28. By September
15 the number had crept up to 149. A total of 146 men (56% of the original
261 men) were recorded as getting sick. Two of those died. No women or children were recorded as dying (unlike later years where they were recorded as dying in equal numbers to the men). At Kingston Mills, 12 men are recorded as having died.
Records for 1830, covering the area from the Isthmus (Newboro) to Kingston Mills, show a total of 1,327 men at the various work sites. Of these, 787 (60%) got sick and 27 (2%) died. In that same reporting period, 13 women and 15 children were also recorded as having died.
In trying to estimate how many people died of malaria, it is a little hard to separate fact from fiction. From a factual perspective, based on Christie’s records, no one died from malaria in 1827, although at least 5 men died of fever. If we look at the sick reports from the period 1828 to 1831, and assume that all the disease deaths during the “sickly season” of August 1 to September 15 were from malaria, then the direct number is about 2% (for the hardest hit area of the southern Rideau). If we simply extrapolate that number over the total workforce of an average of about 2,500 men per year, then from 1828 to 1831, about 200 men died of malaria.
Some have argued that the sick reports only represent deaths at the worksites and don’t take into account people who left the site and died somewhere else. So, if we simply double the number, to take this into account, we get the deaths of about 400 men. However, the bottom line is that we don’t know for sure and never will. It was an equal opportunity killer, the death rates for contractors, tradesmen, labourers and even the Royal Sappers and Miners, appear to have been about the same.
There were 162 Royal Sappers and Miners stationed on the Rideau Canal during the construction period. Of these, 22 died. Of those, only 5 (3%) had their cause of death specifically listed as being “fever ”– the earliest being July 21 and the latest October 15. If we expand the sickly season to cover July 15 to October 30, then we might add two others for which no cause of death was listed, bringing the total to 7 (4.3%). The other deaths included 5 from blasting accidents, 1 by drowning, 1 from apoplexy (a stroke) and 2 from consumption (tuberculosis). The remaining 6 had no cause listed, but they didn’t die during the sickly season.
We do know that the number of deaths attributed to malaria has grown over time, often based on interpretations of general statements or second hand information. For instance, some have interpreted Mactaggart’s “all were laid down together” at Jones Falls and Kingston Mills to mean dead, but he really meant sick. The records indicate that 14 men at those two locations died during the outbreak he described.
The bottom line is that many men died during the building of the Rideau Canal, certainly some hundreds, but how many directly from malaria? Was this the main cause of death? From the records we see that in the southern Rideau, the most malaria prone area, about 60% of the men would get sick during the “sickly season” and that between 2 to 4% would die. We also know that the men suffered from a huge number of medical issues that were typical of the day. Outside of Christie’s often-noted bowel issues (diarrhea, indigestion and constipation) these included dysentery, tuberculosis, syphilis, gonorrhea, fevers from viruses and infection, and a host of other illnesses [see “A Grave Revealing” for more information]. Alcohol was also a issue, Christie noted several medical “relapses” due to overindulgence.
So, there is some suggestion that it was a combination of things that led to people dying. Malaria would certainly have been part of the problem, but those who died might already have had an underlying condition with malaria being the last straw.
Getting Rid of Malaria
Today, there are no traces of malaria in Ontario – it’s gone both physically and from the memory of residents of Ontario. So, how did something so pervasive disappear?
It wasn’t due to medical care, certainly not in the early-mid 1800s. During the 1819 outbreak on the Erie Canal, it was noted that a doctor bled the sick, then dosed them with feverwort, snakeroot, green pigweed, Seneca Oil and Jesuit’s Bark. The last item actually had some merit when it came to malaria, Jesuit’s Bark is another name for the bark of the Cinchona tree. This bark contains quinine which is a both a cure and a prophylactic for the malaria parasite.
Pure Quinine was isolated by two French chemists (Pelletier and Caventou) in 1820. This was much more effective against malaria than ground up Cinchona bark. At the time of the building of the Rideau Canal, Quinine was still rare in Canada and quite expensive. Since it was so rare, yet a well known medicine for malaria, Reverend William Bell would send one of his sons to Montreal to meet the ship bringing it over from Europe, in order to secure a supply for the year.
An 1833 publication noted “Quinine is, of course, known to be a sovereign specific; and for more ordinary practise, a teaspoonful of sulphur in a wine-glass of brandy or other spirit, taken two or three times a-day, accompanied by cathartics and moderate nourishing diet, with suitable clothing, generally effect a cure.”
This is one of the more benign descriptions for a malaria cure found in period medical literature. Since no one knew what actually caused malaria, there were all sorts of “cures.” Another common remedy involved dosing the patient with arsenic. The use of the “ague drop” (potassium arsenate) started in the 1700s with expanded use of this and other arsenic formulas to treat malaria (and other diseases) in the 1800s.
Part of the problem was that no one knew what caused malaria. The meaning of the word is “bad air ” and it was generally thought to be caused by vapour emanations from the water. Colonel By was convinced of this, so he had trees cleared at every work station in order to promote the flow of air which he hoped would clear out the malarial vapours.
It wouldn’t be until the late 1800s that it was discovered that the lowly mosquito was the carrier. Up until that time, it was firmly believed to be something “in the air.” The October 31, 1863 edition of The Scientific American provided a detailed, but completely incorrect, explanation regarding the cause of malaria:
Malaria
“This atmospheric poison has been proved to be caused by the decomposition of organized matter, and it exists to some extent everywhere. Vegetation both grows and dies, and in the soil its decomposition goes on at various rates. Soils generally are acidulous ; but a rich, highly-manured, warm soil is alkaline. Where most alkali exists there is a greater facility for the escape of vapors, such as we suppose to be hurtful. The extreme condition of putrescence may be very readily produced in a soil by artificial means ; the use of a little ammonia, for example, more than vegetation will bear. The substances putrefy until the whole becomes fetid in the highest degree. We have then a soil rich in organic matter and undrained : — a swamp of the worst form if the soil be not very poor ; worse, perhaps, than was ever seen in nature. It is artificial malaria. We can, then, produce malaria from the soil by fostering some of its tendencies.
Cold weather tends to produce acidity of the soil, hence malaria is always diminished with a lower temperature. When a warm alkaline soil is washed with water and exposed to the air, decomposition is stopped, and it sends forth less malaria. Drainage is the most effectual method of preventing malaria arising from swampy districts.”
This quote does provide a clue about how malaria was eradicated from Ontario before it was fully understood that mosquitoes were the carrier (the actual malaria parasite was only discovered in 1880 and it was not until 1897 that mosquitoes were proven to be the carrier). No one wanted to be bitten by mosquitoes, so swamps were drained or oiled in the vicinity of growing urban centres. The Anopheles mosquito, a nightbiter, most commonly bit its human victims inside their houses while they were sleeping. People started to put glass on windows and then eventually screens on windows and doors to prevent mosquito entry. And Quinine, by the mid-1800s, was easily available and was being extensively used as a prophylactic against malaria.
All of these changes had the effect of dropping the malaria parasite, P.vivax, below the infection threshold needed to maintain the malaria cycle. The huge drop in the number of mosquitoes that could actually infect a human and the corresponding drop in the number of infected humans, eventually eradicated malaria from Ontario in the late 1800s. In the U.S., the CDC (Center for Disease Control) declared the U.S. free of malaria by the 1950s.
| |
  |
Quinine
Quinine became available in many forms, as a powder and in many types of tonics and healing elixirs (tonic water today still contains Quinine).
Left: Quinine Sulphate bottle, Science Museum, London, photo by Jaron Chubb, A664060. Right: The Medicine Chest
- Tonics, by Dr. Richard Cannon, Antique Bottle And Glass
Collector Magazine.
|
One of the last references to malaria in the Rideau area may be the December 20, 1895 edition of the Perth Courier which reported “John Cameron, late of Brockville, who died on Dec. 12 at the age of 87 years, from malaria, was buried in Smith’s Falls on Friday.”
Can malaria return to the Rideau area? Highly unlikely since it would require a large number of infected humans being bitten by Anopheles mosquitoes (requiring exposure to the mosquito at night) to start a sustaining cycle. There is one example of this happening in England. Soldiers returning after WWI, who were infected with P.Vivax (which they picked up in Greece and India), caused a small outbreak in the north Kent marshes (which were still full of Anopheles mosquitoes), where the soldiers had been sent to convalesce.
Malaria remains a problem in other parts of the world. In the tropics, P. falciparum malaria kills more than a million people a year.

Sources:
Bush, Edward F., The Builders of the Rideau Canal, 1826-32, Manuscript Report 185,
Parks Canada, Ottawa, 1981 - digital edition, DB185, Friends of the Rideau, 2009.
Cameron, Wendy, Sheila Haines, Mary McDougall Maude (eds), English Immigrant Voices: Labourer’s Letters from Upper Canada in the 1830s, McGill-Queen’s University Press, 2000.
Crandall, Dr. Ian, University of Toronto (Malaria Research), per. comm., 2000.
Dobson, M.J. “History of malaria in England” in Journal of the Royal Society of Medicine, Supplement No. 17, Vol. 82, 1989, pp.3-7.
Fallis, A. Murray, “Malaria in the 18th and 19th centuries in Ontario”, Canadian Bulletin on Medical History, 1(2), 1984, pp.25-38.
Fergusson, Adam, Practical Notes Made During a Tour In Canada and a Portion of the
United States in MDCCCXXXI, William Blackwood, Edinburgh & T. Cadelle, London,
1833.
Haller, John S. Jr., American Medicine in Transition, 1840-1910, University of Illinois,
1981.
Mathison, John, Counsel for Emigrants and Interesting Information from Numerous Sources with Original Letters from Canada and The United States, D. Chalmers & Co., Aberdeen, 1834.
Patychuk, Dianne L., Malaria on the Rideau Canal, 1826-32, unpublished B.A. Thesis study, Queens University, 1979.
Scientific American, Vol. IX, No. 18, October 31, 1863.
Skelton, Isabel, A Man Austere, William Bell, Parson and Pioneer, The Ryerson Press, Toronto, 1947.
Stanzell, Jim “Royal Sappers and Miners, Builders of the Rideau Canal 1826-1832” in
Ottawa Branch News, Vol. 40, No. 4, pp.199-202. Historical Society of Ottawa, 2007.
Valentine, Jaime, Supplying the Rideau: Workers, Provisions and Health Care During the Construction of the Rideau Canal, 1826-1832, Microfiche Report Series 249, Parks Canada, 1985.
Way, Peter, Common Labour: Workers and the Digging of North American Canals, 1780-
1860, Cambridge University Press, 1993.
Wilson, Thomas, An Enquiry into the Origin and Intimate Nature of Malaria, Henry
Renshaw, London, 1858.
|